One of the hardest things to explain to patients is why human beings are such inefficient reproducers. Mice and rabbits seem to have the corner on this market. It just seems logical that one follicle should produce one egg which ultimately makes one embryo and one healthy baby.
But unfortunately this is not reality. Especially in the context of an IVF cycle, the follicles that grow under gonadotropin stimulation tend to have a very low yield for creating a healthy baby. We do not believe that the gonadotropins themselves make for a poor quality egg. Instead, we just believe that women produce an abnormally high amount of abnormal eggs, even young women and egg donors.
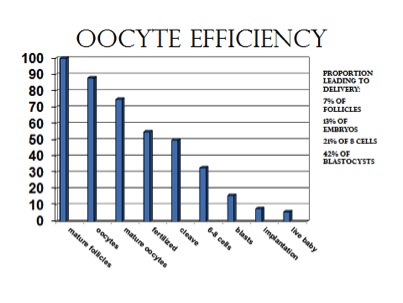
For this reason we try to obtain more eggs knowing that only a small percentage will become healthy embryos for transfer. And at Reproductive Science Center we freeze twice as many embryos as we think will make a healthy baby, knowing that our ability to look at the embryo under the microscope and predict its potential is not perfect.
While it may seem obvious to us in the field, I do not believe this fact is obvious to all patients. Therefore it bears repeating. The follicles that grow in an IVF cycle will not all have a healthy egg. And a healthy-appearing egg does not guarantee a healthy embryo or a baby.
In general, 40 percent of fertilized eggs (day-1 embryos) will be able to be frozen or transferred. Hopefully the knowledge of this fact will help patients understand why they may begin with 15 eggs and only end up with five embryos.
At RSC we still consider five embryos to be a very good yield from a single IVF cycle. Many patients will be able to have one or two children from this single IVF cycle. Remember, it is the quality, not quantity, that matters most: we usually require a high quantity to begin the process with the knowledge that not every egg can become healthy baby.
The above printed graph was presented at a lecture on fertility by Dr. Richard Scott at the Pacific Coast Reproductive Society meeting and was not prepared from RSC data.

Breaking Barriers, Building Families
Since 1983, we have pioneered fertility treatment for every kind of family. We want to help you achieve your dream of having a baby.
Request appointment