Success rates: what are the odds?
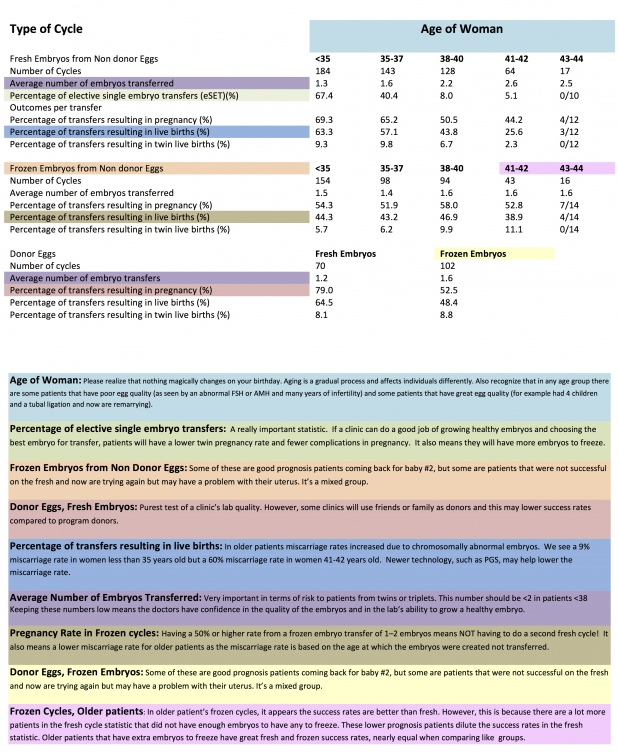
Once a couple become patients at a fertility clinic, what are the odds they will someday take home a live baby? The answer depends on several factors, including the woman’s body, the man’s body, the clinic’s success rate, and luck. Below is a more detailed look at the influences. Click on the image for a larger view:
Physiological factors for success
Consider your own conditions when looking at clinic success rates for any procedure. If you have many of the positive factors on your side and no negative factors, your probability of a successful pregnancy is higher. Of course, a high number of negative factors gives you poorer chances.
Positive factors:
- Younger age of woman (age is not relevant with donor egg services)
- Previous pregnancy with IVF
- Non-smoker
Negative factors:
- Age – the older a woman, the less likely she will become pregnant (age is not relevant with donor egg services)
- History of recurrent miscarriage
- Both male and female partner infertility
- Previous history of assisted reproduction (three or more cycles) without success
- Uterine abnormality (DES, fibroids)
- Certain types of ovarian dysfunction (high FSH level)
- Hydrosalpinx – an excessive dilation and fluid accumulation in the fallopian tube.

Breaking Barriers, Building Families
Since 1983, we have pioneered fertility treatment for every kind of family. We want to help you achieve your dream of having a baby.
Request appointmentMeasuring clinic success rates
Fertility clinics use several ways to measure success, depending on which stage of treatment the couple reaches. For that reason, published success rates can be misunderstood and misleading in comparing clinics. The best picture of a clinic’s success comes from examining the pregnancy rates for all three stages of treatment.
Even these statistics do not tell you exactly what you want to know – the number of women who ultimately take home a baby based on the number of women who start treatment. Tip: ask each clinic whether its statistics refer to cumulative cycle data or current cycle data. And always ask for documentation and a breakdown of the data by age, so that you can compare the statistics to your own situation.
The third column in the table below gives an example of varying success rates that a clinic would report for each measurement.
| Measurement | Calculation |
Example |
| Clinical Pregnancy rate per cycle initiation | Total pregnancies/Number of women who start ART treatment | 15% (15/100) |
| Clinical Pregnancy rate per retrieval | Total pregnancies/Number of women who have eggs retrieved | 19% (15/80) |
| Clinicial Pregnancy rate per Transfer | Total pregnancies/Number of women who have an embryo transfer | 25% (15/60) |
| Delivery Rate per Transfer | Total deliveries/Number of women who have an embryo transfer | 16% (10/60) |
Example and explanation
Let’s take an example of a clinic that initiated 100 cycles–they started 100 women on an ART procedure by prescribing fertility hormones to stimulate multiple egg production. Some women will be counted in more than one cycle.
Of those women, 20 responded poorly to the fertility drugs and ended the cycle, and 80 responded well and proceeded to egg retrieval. In a retrieval, the physician removes eggs from the woman’s ovaries. Physicians cancel some cycles before retrieval — usually because the woman responds poorly to fertility drugs and does not develop enough eggs.
Of the 80 egg retrievals, 20 women did not have enough eggs to fertilize and develop properly into embryos for an embryo transfer. The transfer is the final IVF treatment stage, in which the physician transfers embryos into the woman’s uterus.
Of the 60 women who did have an embryo transfer, 15 became pregnant.
Of those same 60 women, 5 lost the pregnancies to miscarriage or other problems, and 10 gave birth.
Therefore, the percentage of women who took home babies after starting an ART cycle (for this fictitious sample clinic) is 10 percent.
Comparing clinic success rates
In addition to statistics on the Web site of the Centers for Disease Control and Prevention, the Society for Assisted Reproductive Technology (SART) collects data from fertility clinics across the U.S. The SART statistics allow you to compare different fertility clinics. The CDC’s Web site also explains how to read a fertility clinic’s statistics table.
NOTE: “A comparison of clinic success rates may not be meaningful because patient medical characteristics, treatment approaches and entrance criteria for ART may vary from clinic to clinic.”
SART statistics
A program’s success rate depends upon the quality of its laboratory, practitioners, and staff. It also depends on factors beyond the program’s control, such as physiological factors that include the age of the patients and the cause of infertility.
Evaluating a clinic’s success with hormone treatments and surgery is difficult because of the unique conditions and treatment of each patient and the lack of standardized data collection.
You can compare Assisted Reproductive Technology (ART) services by examining each clinic’s statistical data. Be sure to compare similar statistics, since fertility clinics calculate success rates in different ways.
Which ART?
The ART procedures that a clinic uses may reveal more information about its experience. Recent studies have shown that IVF can be as successful as the theoretically superior, but more invasive procedures of GIFT and ZIFT. These studies support the idea that excellent embryology laboratories can have pregnancy rates for IVF equal to or better than those for GIFT and ZIFT. Laboratories that can maintain high rates with IVF will usually choose it over GIFT and ZIFT procedures.
About SART/CDC statistics
Most U.S. fertility programs follow the guidelines of the Society for Assisted Reproductive Technology (SART) to report success rates. Each year, SART and the Centers for Disease Control and Prevention (CDC) collect and publish this comprehensive, clinic-specific data. Results are organized by state and by procedure. The data includes information on pregnancy outcomes, such as the rate of miscarriages, twins, and other multiple births.
The most current national report of fertility clinic success rates is on the SART Web site, based on ART procedures performed in 2004. The CDC’s web site includes an explanation of how to read a fertility clinic’s statistics table.
You can request more recent SART reports directly from each fertility clinic that you are considering. Also, ask for reports from previous years to look for trends in the data over time. Year-to-year data can reveal information on the quality, stability, and experience of the program. It’s a good idea as well to ask each clinic to provide its most recent SART statistics for your age based on delivery rate per embryo transfer.